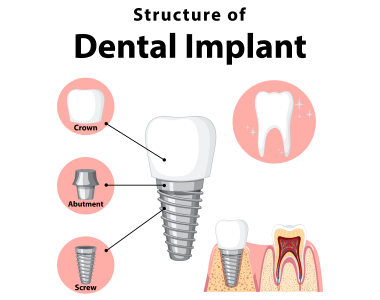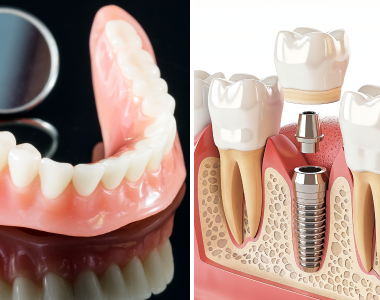
When it comes to replacing missing teeth, two of the most common options are dental implants and dentures. While both offer a solution for tooth loss, dental implants have become the preferred choice for many due to their numerous benefits. In this blog, we will explore the advantages of dental implants over dentures and why they might be the better option for restoring your smile and oral health.
1. Superior Comfort and Stability
One of the most significant advantages of dental implants is their comfort and stability. Unlike dentures, which can shift and cause discomfort, implants are securely anchored in the jawbone. This eliminates the worry of slippage while eating or speaking. The stability provided by dental implants ensures a more natural feel and allows you to enjoy your favorite foods without concern.
2. Improved Chewing and Speech
Dentures can sometimes make it difficult to chew certain foods or speak clearly. Dental implants, on the other hand, function just like natural teeth. With implants, you can chew food comfortably, and your speech remains clear and unaffected. This is because the implants fuse with your jawbone, providing the same level of stability as your natural teeth.
3. Long-Lasting Solution
While dentures may need adjustments, relining, or even replacement over time, dental implants offer a long-lasting and durable solution. With proper care and regular dental check-ups, implants can last a lifetime. This makes them a more cost-effective option in the long run compared to dentures that may require frequent upkeep.
4. Preservation of Jawbone Health
One of the most critical benefits of dental implants is their ability to preserve the jawbone. When you lose a tooth, the underlying bone can begin to deteriorate over time due to lack of stimulation. Dental implants help maintain bone density by stimulating the jawbone, preventing bone loss. Dentures, however, do not offer this benefit, which can lead to bone shrinkage and facial sagging over time.
5. Natural Appearance and Feel
Dental implants are designed to look and feel like natural teeth. They are custom-made to match the color, shape, and size of your surrounding teeth, resulting in a seamless appearance. Dentures, while functional, often have a more artificial look. Dental implants provide a more aesthetic and natural-looking smile, boosting your self-confidence and overall satisfaction.
6. No Adhesives or Removal
With dentures, adhesives are often required to keep them in place, which can be messy and inconvenient. Dental implants are a permanent fixture in your mouth, eliminating the need for any adhesives. There’s also no need to remove them at night for cleaning, unlike dentures, which require regular removal and soaking.
7. Better Oral Health
Unlike dentures, which may trap food particles and bacteria, dental implants integrate naturally with your gums and jawbone. This makes it easier to maintain proper oral hygiene, reducing the risk of gum disease or other oral health issues. Implants do not negatively impact neighboring teeth, unlike certain types of dentures or bridges.
Conclusion
While dental implants and dentures replace missing teeth, dental implants provide superior comfort, durability, and long-term benefits. From preserving jawbone health to offering a more natural appearance, implants are an excellent solution for restoring function and aesthetics. If you are considering tooth replacement options, consult your dentist to determine if dental implants are the right choice.


 Review Us
Review Us Review Us
Review Us